Dr James Thambyrajah Uses Case Studies to Illustrate Four Different Types of Skin Lesion and Describes How Each Condition Should be Managed in Primary Care
| Read This Article to Learn More About: |
|---|
|
Skin lesions are a frequent presentation in general practice so it is important for clinicians to be able to distinguish benign conditions from those such as melanoma that will require urgent referral and treatment. The majority of skin lesions referred urgently via 2-week wait referrals for suspected skin cancer are found not to be malignant, indicating that there is a need for better recognition of non-malignant skin lesions in primary care.1
A thorough history and examination will help with diagnosing skin conditions and guide the next steps for referral and management. Ask the patient about how long the lesion has been present, if it has grown and/or changed in shape, if there is any associated pain, and if it bleeds or oozes. Any past medical history or family history of skin cancer should be identified.2
A systematic examination of the lesion based on the history will help with diagnosis and ensure that serious conditions such as melanoma can be ruled out. If the diagnosis is uncertain, particularly if symptoms are not typical, then the clinician may want to discuss the signs and symptoms with a specialist to decide whether a referral is required.3
Red Flags
Around 13,000 melanomas are diagnosed every year in the UK, which means the average GP is likely to encounter a melanoma once every 3 to 5 years. NICE recommends referring patients urgently via a 2-week suspected cancer pathway for melanoma if a suspicious pigmented skin lesion scores 3 or more using the weighted 7-point checklist (see Box 1).3
| Box 1: Weighted 7-Point Checklist for Melanoma3 |
|---|
© NICE 2016. Skin cancers—recognition and referral. NICE Clinical Knowledge Summary. cks.nice.org.uk/skin-cancers-recognition-and-referral All rights reserved. Subject to Notice of rights. NICE guidance is prepared for the National Health Service in England. All NICE guidance is subject to regular review and may be updated or withdrawn. NICE accepts no responsibility for the use of its content in this publication. |
The following case studies aim to illustrate the classic features of some common skin lesions and how to manage and refer as appropriate.
Case 1
A 68-year-old man presents with a small lesion on his right cheek, which he says has been there for several weeks. It is a firm lesion which is dry, red, and does not bleed.
Diagnosis
The diagnosis is basal cell carcinoma (BCC) (see Figure 1). BCCs are the most common form of skin cancer, accounting for around 80% of all skin cancers. People with white skin have a lifetime risk of 20–40% of having a BCC.4 Around 75,000 BCCs are diagnosed every year in the UK, which means the average GP is likely to diagnose one BCC per year. BCCs are very rarely fatal but early diagnosis is important to avoid extensive and potentially disfiguring treatment.3
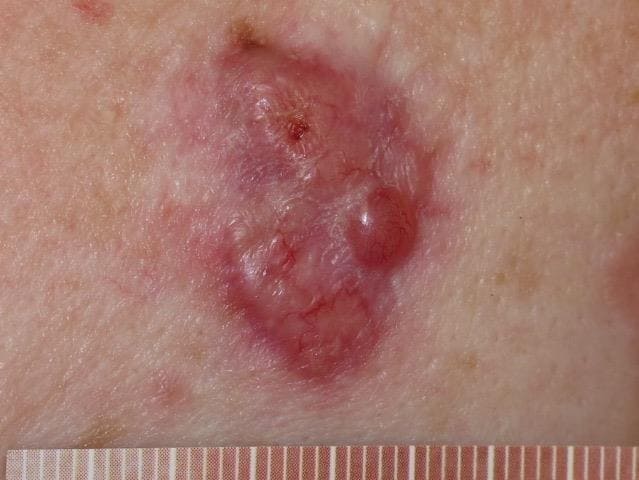
Source: DermNet NZ
Reproduced with permission
Known risk factors for BCC include exposure to ultraviolet light, increasing age, having fair skin that burns easily, immunosuppression, smoking, trauma, previous BCCs, and Gorlin syndrome. Sun-exposed areas, particularly on the head and neck, are most commonly affected but BCCs can occur on any part of the body. Patients may have more than one BCC so it is important to examine their skin thoroughly.4,5
BCCs are often slow growing, vary in size and appearance, and may exhibit spontaneous bleeding, scabbing, or ulceration. They are not usually painful. They may be skin-coloured, pink, or pigmented, but the appearance will vary according to the type of BCC (Table 1). While it might be possible to diagnose a BCC visually, excision biopsy is often used to confirm the diagnosis.1,3–5
Table 1: Different Types of BCC1
| Common Location | Features | |
|---|---|---|
| Nodular | Face | Cystic, pearly, telangiectasia May be ulcerated Micronodular and microcystic types may infiltrate deeply |
| Superficial | Upper trunk and shoulders Often multiple | Erythematous well-demarcated scaly plaques, often >20 mm Slow growth over months or years May be confused with Bowen’s disease or inflammatory dermatoses |
| Morphoeic (or sclerosing or infiltrative) | Mid-facial sites | Skin-coloured, waxy, scar-like Prone to recurrence after treatment May infiltrate cutaneous nerves |
| Pigmented | Brown, blue or greyish lesion Nodular or superficial histology May resemble malignant melanoma | |
| Basosquamous | Mixed BCC and squamous cell carcinoma Potentially more aggressive than other forms of BCC | |
| © NICE 2010. Improving outcomes for people with skin tumours including melanoma (update)—the management of low-risk basal cell carcinomas in the community. Cancer Service Guideline 8. www.nice.org.uk/guidance/csg8 All rights reserved. Subject to Notice of rights. NICE guidance is prepared for the National Health Service in England. All NICE guidance is subject to regular review and may be updated or withdrawn. NICE accepts no responsibility for the use of its content in this publication. | ||
| BCC=basal cell carcinoma | ||
Management
NICE recommends routine referral for skin lesions suspected to be BCCs; however, if the clinician is concerned about factors such as lesion site or size relating to a suspected BCC, then an urgent 2-week cancer referral may be appropriate.3 The Primary Care Dermatology Society recommends that basosquamous BCCs should also be referred urgently.4
Most BCCs will be removed using superficial skin surgery or cryotherapy, with other methods including photodynamic therapy and radiotherapy. However, superficial BCCs can often be managed medically without the need for surgery.1
Clinical Outcome
The patient’s BCC was surgically removed via excision and primary closure. Histology confirmed a ‘nodular basal cell carcinoma reaching the reticular dermis’.
Case 2
An 80-year-old woman presents with a lump on her right shoulder, which she has had for approximately 2 weeks. She describes it increasing in size. She has always lived in the UK and describes her skin as ‘burning easily’ on exposure to the sun.
Diagnosis
The diagnosis is squamous cell carcinoma (SCC)—the second most common form of skin cancer (see Figure 2). Around 25,000 SCCs are diagnosed every year in the UK, which means the average GP is likely to diagnose one every 1 or 2 years.3
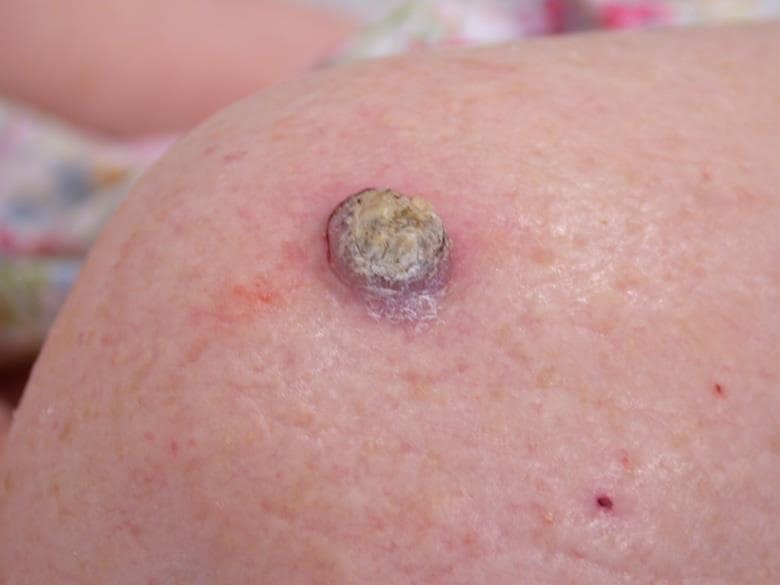
Source: DermNet NZ
Reproduced with permission
SCCs share many risk factors with BCCs, with the addition that patients who have had a transplant and are taking immunosuppressants are more prone to developing SCCs and these lesions can be aggressive. The backs of hands, forearms, upper face, lower lip, and the ear are common sites and they can also be found in areas of chronic inflammation, such as leg ulcers. SCCs occur most frequently in older patients but they may be found in younger patients who have xeroderma pigmentosum, albinism, or epidermolysis bullosa.6
SCCs grow more quickly than BCCs and tend to be painful or be associated with sensory changes. A characteristic sign of SCCs is induration and the tissue around the lesion may appear inflamed. As with BCCs, the diagnosis will usually be confirmed with excision biopsy.3,6
Management
NICE recommends that suspected SCCs should be referred via the 2-week suspected cancer pathway.3
Although most SCCs can be treated successfully, they can occasionally metastasise.6 Larger and deeper SCCs are more likely to metastasise, as are poorly differentiated tumours.7
Cutaneous SCCs are nearly always managed by surgical excision, including Mohs micrographic surgery if possible, which is associated with a lower local recurrence rate than other treatments. SCCs will be excised with a margin of around 4–10 mm depending on the size of the lesion to ensure that the whole tumour is removed. Skin grafts or flaps may be needed to repair the defect. Alternative methods of removal include curettage and electrocautery, cryotherapy, and radiation therapy.7
Most SCCs are cured by treatment. About 50% of patients at high risk of SCC develop a second one within 5 years of their first lesion. They are also at increased risk of other skin cancers, especially melanomas.8
It is worth noting the importance of educating the patient regarding regular self-skin examinations, and longer annual skin checks.8
Clinical Outcome
The patient had her lesion examined with a dermatoscope and features were found to be consistent with an SCC. This patient’s lesion was removed via minor surgery with 4 mm margins. Histology confirmed a keratoacanthoma-like well differentiated stage pT1 SCC.
Case 3
A 34-year-old woman presents with a 4 mm lesion on her left thigh that has been present for several months. It is firm, solid, and painless. She does not believe it has increased in size.
Diagnosis
The diagnosis is dermatofibroma (see Figure 3). Dermatofibromas are common benign fibrous nodules that often occur on the thighs and lower legs. They are more common in females and in young adults.9
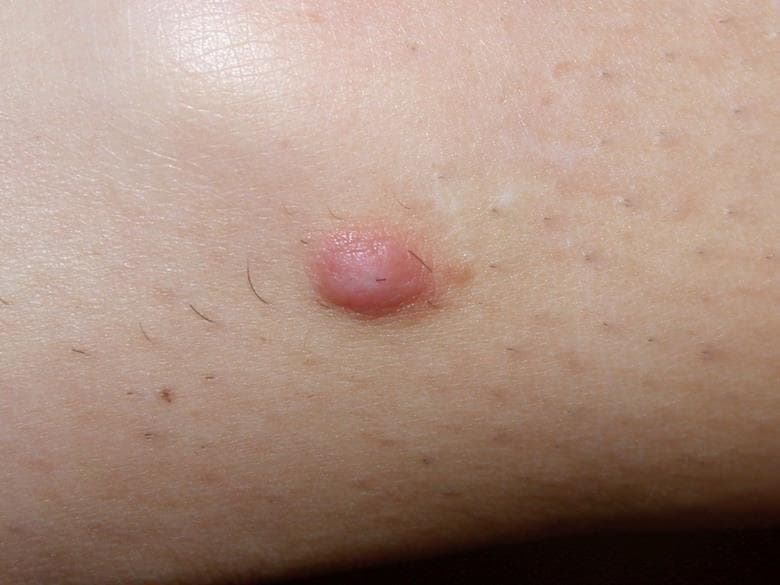
Source: DermNet NZ
Reproduced with permission
People may have one or multiple lesions. They vary in size but most are around 5 mm and slightly elevated, though they can be larger. They occur as firm nodules that dimple in the middle when the skin is pinched. They are often red or light brown and are normally asymptomatic but they can be painful if knocked.9
Management
Dermatofibromas do not normally require treatment; however, they are occasionally removed when the diagnosis is uncertain or if causing undue discomfort. Treatment is by surgical excision, with all specimens sent for histology.9
Clinical Outcome
The patient was told by her GP after clinical examination that this skin lesion was a dermatofibroma. She was given a patient information leaflet about the condition and was reassured and told to come back if the lesion changed in shape or colour.
Case 4
A 75-year-old man comes back for a check up for a large, dark brown mole on his back that has grown bigger over the last 12 months. He said he wouldn’t have come to the surgery but his wife was concerned.
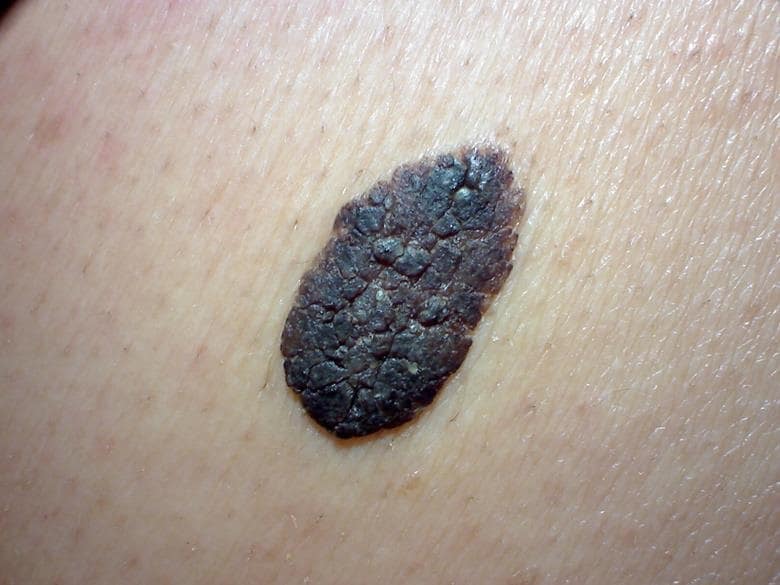
Source: DermNet NZ
Reproduced with permission
Diagnosis
The diagnosis is seborrhoeic keratosis (see Figure 4). Seborrhoeic keratoses are common benign lesions that present as people get older. They are frequently found on the trunk and face and can occur in large numbers. They are usually brown or black, though can be paler, and therefore when highly pigmented may resemble malignant lesions.10
They often look as if they are greasy and have a ‘stuck-on’ appearance. They are typically 1–3 cm in diameter, although they can be larger. Sometimes they exhibit the Leser-Trélat sign, which is the sudden occurrence of multiple seborrhoeic keratoses.10
Management
Most seborrhoeic keratoses do not need any treatment. However, if there is any doubt about diagnosis, it is recommended to refer under the 2-week rule. If removal is desired, then the management options are cryotherapy, curettage, and cautery, with samples sent for histology.10
Treatment Outcome
After clinical examination by his GP, the patient was told that the lesion was a seborrhoeic keratosis. He was reassured and was told to come back if the lesion changed in shape or colour.
Conclusion
Skin lesions are a common presentation in primary care, many of which can be diagnosed based on history and clinical examination. The challenge for GPs is in distinguishing between benign and malignant lesions, so that only those that require urgent review and treatment are referred under the 2-week wait.
Dr James Thambyrajah
Full-time salaried GP, Cheam Family Practice, Sutton

