Dr Jennifer Parkhouse Unravels Four Case Studies Covering Several Diagnoses of Childhood Rashes and Explains How Each Condition Should be Managed in Primary Care
| Read This Article to Learn More About: |
|---|
|
Rashes in children are common and as a consequence are a familiar consultation in general practice. They can vary from simple and benign conditions to life-threatening disease, such as meningitis. The following case studies aim to look at some of the common childhood rashes seen in general practice and how they are subsequently managed.
Case 1
A 5-year-old boy is brought into the surgery. He is normally fit and well but his mother has noted a cluster of spots in his right armpit that have been present for a few weeks. She made an appointment as she noticed some redness around the spots as well. On examination, the spots are firm, raised, and have a little dimple in the middle.
Diagnosis
The diagnosis here is molluscum contagiosum—a common skin condition caused by a member of the poxvirus family.1 There are at least four viral subtypes. It mainly affects children under the age of 10 years, and the infection can spread in several ways, including direct skin-to-skin contact, indirect contact (e.g. sharing towels), and autoinoculation (e.g. scratching).2
The molluscum contagiosum virus causes characteristic skin lesions that appear as single, or often multiple, dome-shaped papules (see Figure 1).3 The papules range from 1–6 mm and may be white, brown, or pink. They often have a waxy and shiny look with a central pit. The number of papules can vary from a few to hundreds. Mollusca frequently induce dermatitis around them, which can become itchy and pink. As the papules resolve they may become inflamed or scabby for a week or two. They tend to be found in warm, moist places such as the armpit, groin, genital areas, and behind the knees, but do not occur on palms or soles.2
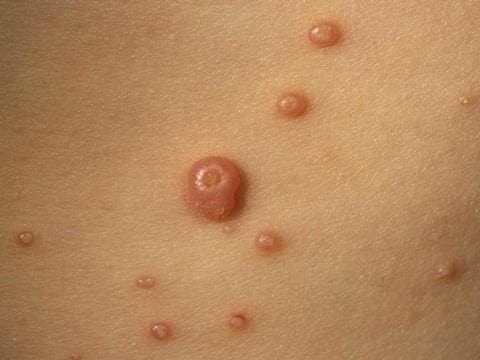
Source: Prof Raimo Suhonen, DermNet NZ.
Reproduced with permission.
Diagnosis is generally elucidated by clinical examination, looking for the characteristic papules. Diagnosis may occasionally be made on skin biopsy.
Management
The lesions will typically resolve within 1–2 years and do not usually cause symptoms.4 In children, about 50% of cases clear after 12 months and two-thirds after 18 months.2 A Cochrane review determined that no single intervention had been shown to be convincingly effective,5 so treatment is not usually recommended in primary care.4 Complications can arise and should be treated; these include:2
- secondary infection
- conjunctivitis (if the eye is involved)
- disseminated secondary eczema
- scarring due to surgery.
General advice is to reassure that molluscum contagiosum is a self-limiting condition, and to avoid squeezing/scratching the lesions and sharing towels, clothing, and baths. Eczematous complications can be common, especially in children with atopy, and should be treated promptly. Itching should be managed with an emollient or a mild steroid, and infection should be managed with topical fusidic acid 2%.4
Physical treatments include cryotherapy, picking out the central white core, curettage, and laser ablation. Medical treatments include antiseptics (e.g. hydrogen peroxide cream), cantharidin solution, podophyllotoxin cream, and wart paints such as salicylic acid. Imiquimod and sinecatechins are also sometimes used but both are unproven.2 (NB at the time of publication [December 2018], imiquimod was not licensed for molluscum contagiosum; the prescriber should follow relevant professional guidance, taking full responsibility for all clinical decisions. Informed consent should be obtained and documented. See the General Medical Council’s guidance on Good practice in prescribing and managing medicines and devices6 for further information.) If the patient is immunocompromised (in these cases the mollusca can take years to clear), if the mollusca are extensive and painful, or if there is diagnostic uncertainty, the patient should be referred to a dermatologist for advice and treatment. See the NICE Clinical Knowledge Summary on molluscum contagiosum for further details.4
Clinical Outcome
The boy’s mother was reassured that molluscum contagiosum is self-limiting, and was advised to leave the spots alone. The boy was given a mild steroid (hydrocortisone 1%) to help settle the localised dermatitis. The spots cleared within 1 year.
Case 2
A 3-year-old girl presents with a high temperature, which started 2 days ago. She has been off her food and her parents have brought her in because they have just noticed some small red spots around her mouth, hands, and her nappy area. Some of the spots have started to blister.
Diagnosis
The diagnosis is hand, foot, and mouth (HFM) disease—a common viral infection. It tends to affect children younger than 5 years, but can occur at any age.7 The disease is highly infectious so several members of a family or school class can be affected.8
Hand, foot, and mouth disease is caused by viruses belonging to the enterovirus group, including coxsackieviruses, echoviruses, polioviruses, and other enteroviruses.7 It is caused primarily by coxsackie A16 and enterovirus 71.9 It usually causes a mild, self-limiting disease; however, HFM caused by enterovirus 71 has been associated with serious complications involving the central nervous system (CNS).10
HFM typically starts with a fever, sore throat, and reduced appetite, followed by a rash 1–2 days later. The rash usually develops as small red spots, often in the back of the mouth or on the tongue, which then blister and can become painful (see Figure 2). A skin rash on the palms of the hands and soles of the feet may develop as flat red spots, which will sometimes blister (see Figure 3). The rash may also appear on the knees, elbows, buttocks, and genital area.7
A diagnosis of HFM is generally made clinically, owing to the characteristic appearance of blisters in the typical sites (hands, feet, and mouth).8
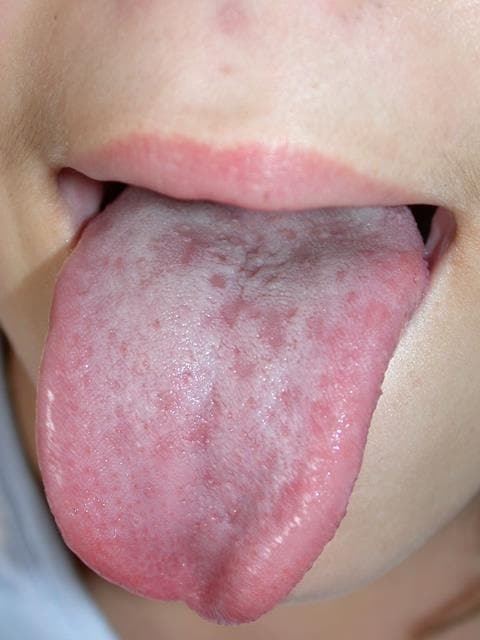
Source: DermNet NZ
Reproduced with permission
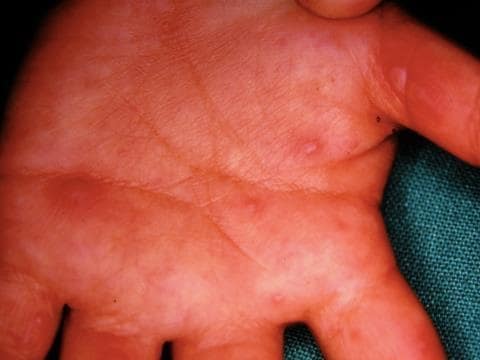
Source: DermNet NZ
Reproduced with permission
Management
Specific treatment is not required. The child should be encouraged to maintain adequate fluid intake to prevent dehydration—topical analgesia (e.g. benzydamine hydrochloride spray) can be given to alleviate oral pain if necessary. The blisters are infective until they have dried up (this is usually within a few days) and stools can be infective for up to 1 month.8 If dehydration or involvement of the CNS is suspected, then hospital admission should be organised.11
Clinical Outcome
The 3-year-old girl continued to be off her food for several days but responded well to the use of a topical benzydamine hydrochloride spray, which numbed the pain enough for her to maintain her fluid intake. Her younger sister also caught the virus, but both children fully recovered within a week.
Case 3
New parents bring in their 6-month-old boy who has had a sore bottom for the past week. He has recently experienced gastroenteritis and has passed a lot of loose stools. His parents say that he is crying a lot when he has his nappy changed and the antiseptic cream they normally use has not helped. He has not had any skin problems prior to this.
Diagnosis
The diagnosis is napkin dermatitis—the most common dermatological condition in infants, predominantly affecting those aged 3–15 months.12,13
Napkin dermatitis follows damage to the normal skin barrier and is a form of irritant contact dermatitis (see Figure 4).13 Primary factors that can cause napkin dermatitis include skin maceration (caused by prolonged contact with urine or faeces/diarrhoea), friction, and poor skin care.12 Other causes include Candida albicans, impetigo, atopic eczema, psoriasis, seborrhoeic dermatitis, and miliaria.13
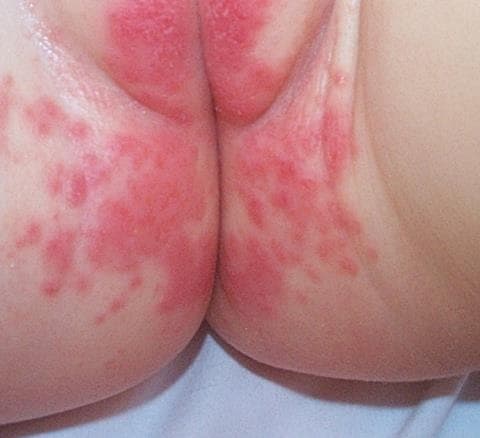
Source: DermNet NZ
Reproduced with permission
Management
The NICE Clinical Knowledge Summary on Nappy rash provides a clear approach to management.14 Self-management strategies include using higher absorbency nappies, leaving nappies off for as long as possible (to help the skin dry), and cleaning the skin every 3–4 hours or as soon as wetting/soiling occurs.14
If there is mild erythema and the child has no other symptoms then an over-the-counter barrier preparation such as nappy rash ointment, zinc and castor oil, or white soft paraffin can be used. Remember to advise parents to apply it thinly at each nappy change as a thick layer can cause water retention and worsen the symptoms.14
If the affected skin is inflamed and causing discomfort, then a mild topical steroid such as 1% hydrocortisone can be used underneath the barrier cream—advise parents to apply the hydrocortisone first and wait a few minutes before applying the barrier preparation.14
If a Candida infection is suspected, then a swab should be taken to confirm and an imidazole cream prescribed. If a bacterial infection is suspected, prescribe flucloxacillin/clarithromycin for 7 days and confirm the infection with a swab. If the rash is not responding as expected, check adherence to treatment, adjust the choice of antibiotic if indicated on swab results, and consider speaking to a microbiologist or referring the patient to a dermatologist.14
Clinical Outcome
The parents were initially advised to use some specific nappy ointment cream instead of the usual antiseptic cream. This led to a slight improvement but as there was still significant redness, hydrocortisone was prescribed, which quickly settled the rash. The infant has not had any symptoms since.
Case 4
A 7-year-old girl attends the GP practice with a rash. She has had a flu-like illness for the past few days and a sore throat. The rash appeared a couple of days later and is pinkish red and is slightly rough to touch. On examination, her tongue is notably red and swollen.
Diagnosis
The diagnosis is scarlet fever. Scarlet fever is an infection caused by the toxin-producing strains of Streptococcuspyogenes (also known as group A strep).15 It is usually a mild, self-limiting illness that commonly affects children between the ages of 5 and 15 years.16 In the UK it is a notifiable disease.
Scarlet fever will only develop in individuals who are susceptible to the toxin produced by the bacteria. Therefore, it is possible that two children in the same family may have the streptococcal infection but only one (who is susceptible to the toxin) goes on to develop scarlet fever.17 The first symptoms of scarlet fever often include a sore throat, headache, fever, nausea, and vomiting. After 12–48 hours the characteristic red rash develops.18
Scarlet spots or blotches are often the first sign of the rash. As it progresses it starts to look like sunburn with goose pimples, and the skin may have a rough sandpaper feel.17 The rash typically first appears on the chest and stomach, before rapidly spreading to the other parts of the body.18
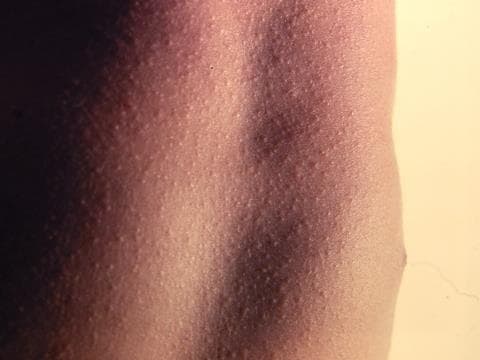
Source: DermNet NZ
Reproduced with permission
Around day 6 of the infection, the rash starts to fade and peeling occurs—this can last up to 6 weeks.17 The child may also get a white coating of the tongue, which peels after a few days leaving the characteristic strawberry tongue appearance.18
Management
If scarlet fever is suspected and the child is well and not requiring admission, then prescribe antibiotics. A 10-day course of phenoxymethylpenicillin (four times a day) should be prescribed first line. Amoxicillin can be given if the patient is unable to swallow tablets or if compliance to penicillin is a concern. For patients with an allergy to penicillin, prescribe azithromycin once a day for 5 days. Public Health England should be notified once a working diagnosis is made. Symptoms do not normally last longer than a week and antibiotics should help prevent any complications. The child should stay away from school or nursery for 24 hours after starting antibiotics.19
Clinical Outcome
The patient started to feel better after the first 3 days of the antibiotics. She took the full course and has been well since.
Dr Jennifer Parkhouse,
GP, Harrogate, GPwSI in Paediatrics

