Dr David Stephens Summarises New Recommendations from the Updated SIGN Guideline on the Management of Osteoporosis and Prevention of Fragility Fractures
| Read This Article to Learn More About: |
|---|
Find key points and implementation actions for STPs, ICSs, and clinical pharmacists in general practice at the end of this article |
Osteoporosis is a disease of bone formation that results in a reduction in the strength of bones and predominantly presents as fragility fracture in older women.1,2 Osteoporosis is caused by the microarchitectural deterioration of bone tissue, which leads to low bone mass and an increased risk of fractures.1,3 The condition is normally diagnosed by measuring bone density via dual-energy X-ray absorptiometry (DXA) scanning and calculation of a patient’s T-score, which equates to the difference in mean bone density between the patient and a healthy young woman.1,4 A diagnosis of osteoporosis can be made at 2.5 standard deviations below the mean bone density of a healthy young woman (T-score ≤ –2.5).1,5,6
It is estimated that around 180,000 fractures occur as a result of osteoporosis in England and Wales each year.7 Osteoporosis is thought to have similar morbidity to a range of other chronic non-communicable diseases, such as rheumatoid arthritis, asthma, and hypertension-related heart disease, but has a lower profile when it comes to diagnosis and treatment.8 People with hip fracture are at high risk of future fracture1 and have a high mortality—about 6% of people with a hip fracture die within 30 days.9
SIGN 142 on Osteoporosis and Fragility Fractures
The Scottish Intercollegiate Guidelines Network (SIGN) has recently updated SIGN 142, first published in March 2015.1 The 2020 update includes new evidence on HIV as a risk factor and discussion of trials in targeting treatment through population screening. Sections on the use of pharmacological therapies zoledronic acid, denosumab, and parathyroid hormone have been updated, and a new section on romosozumab has been included. Recommendations for use of risedronate and zoledronic acid in men have also been added.
Although younger women and men can develop osteoporosis—especially those with certain characteristics (for example, a sedentary lifestyle, history of smoking, or high alcohol intake) or who take specific medications (for example, corticosteroids, proton pump inhibitors, and some sedatives)—the main group of patients with osteoporosis or a history of fragility fracture is women after the menopause.8 The update to SIGN 142 includes a revised algorithm that summarises the pathway for the assessment and treatment of postmenopausal women (see Figure 1).1
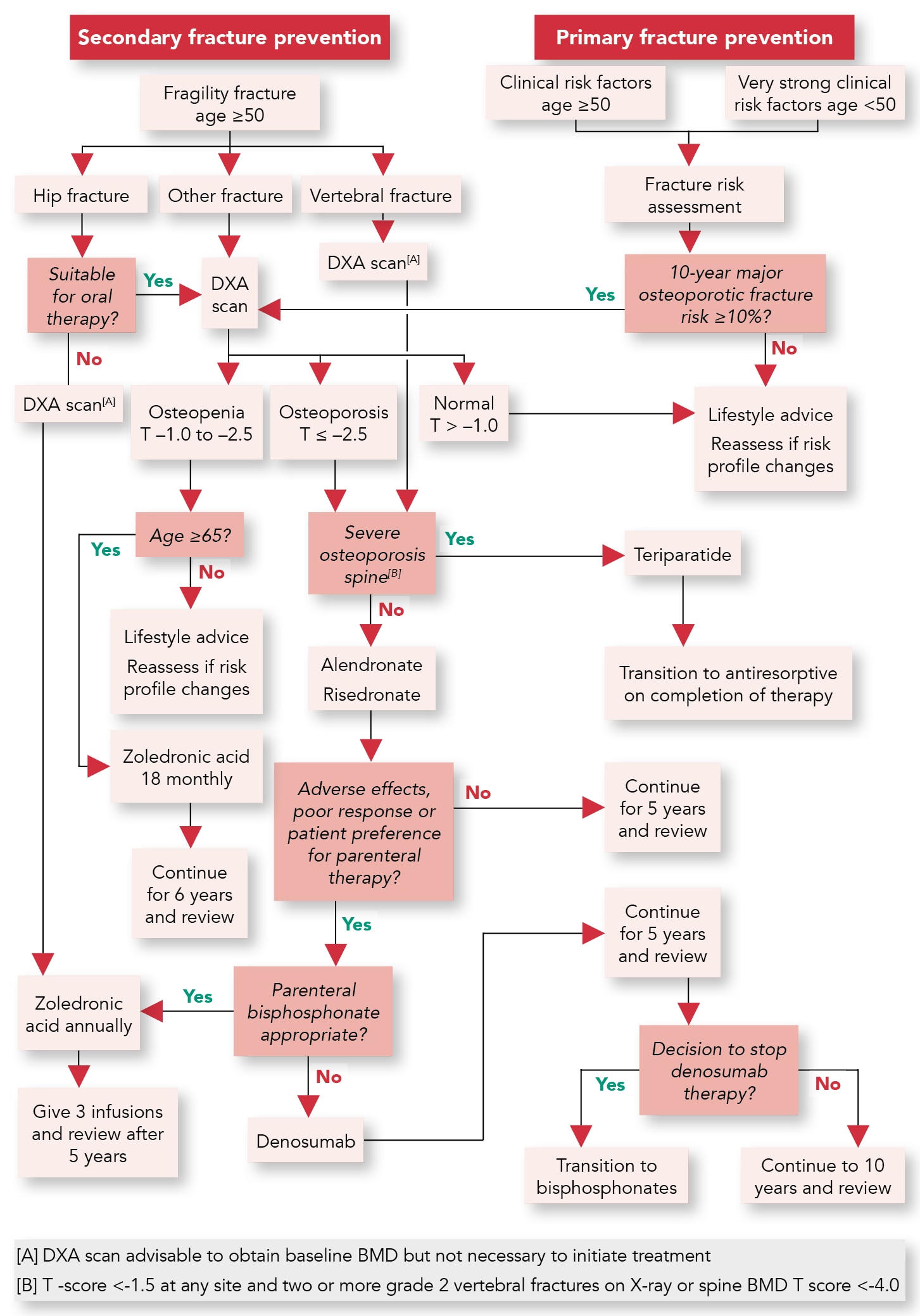
Scottish Intercollegiate Guidelines Network. Management of osteoporosis and the prevention of fragility fractures. SIGN 142. Edinburgh: SIGN, 2015 (updated 2020). Available at: www.sign.ac.uk/our-guidelines/management-of-osteoporosis-and-the-prevention-of-fragility-fractures/
Reproduced with permission.
BMD=bone mineral density; DXA=dual-energy X-ray absorptiometry
Presentation and Assessment
Osteoporosis is initially asymptomatic and often remains undiagnosed until a fragility fracture occurs.7 There are mainly two ways in which patients with osteoporosis present. Some patients present with a fragility fracture, which is often caused by mechanical forces that would not normally result in fracture (low-level trauma);1 these are commonly wrist or hip fractures. Patients can also present with vertebral fractures, which manifest acutely as severe back pain or asymptomatically on magnetic resonance imaging scanning or spinal X-ray.10
Fracture-risk assessment should be carried out, preferably using QFracture®, followed by a DXA scan if the patient has clinical risk factors for osteoporosis and anti-osteoporosis treatment is being considered.
Fracture-risk assessment should also be considered for people presenting with previous fractures, coexisting conditions, long-term use of certain drug therapies, or lifestyle risk factors, such as smoking (see Table 1).
Postmenospausal women who have experienced recent vertebral or hip fracture who cannot or are unwilling to take oral bisphosphonates may be started on treatment without bone mineral density (BMD) measurements, if obtaining the measurements is felt to be impractical.
Risk Factors for Osteoporosis
The SIGN guidance divides risk factors into non-modifiable, modifiable, coexisting diseases, and drug therapy (see Table 1). The update to SIGN 142 includes advice that people living with HIV are at increased risk of fracture and should be considered for a risk assessment. This advice is particularly important for those with several risk factors.1
Table 1: Risk Factors Associated with Fragility Fracture Which Should Prompt Consideration of Fracture-risk Assessment1
| Risk Category | Causative Factor |
|---|---|
| Non-modifiable risk factors | previous fracture |
| parental history of osteoporosis | |
| history of early menopause (below age of 45) | |
| Modifiable risk factors | low body mass index (<20 kg/m2) |
| smoking | |
| low bone mineral density | |
| alcohol intake | |
| Coexisting diseases | diabetes |
| inflammatory rheumatic diseases (rheumatoid arthritis or systemic lupus erythematosus) | |
| inflammatory bowel disease and malabsorption | |
| institutionalised patients with epilepsy | |
| human immunodeficiency virus | |
| primary hyperparathyroidism and endocrine diseases | |
| chronic liver disease | |
| neurological diseases (including Alzheimer’s disease, Parkinson’s disease, multiple sclerosis, stroke) | |
| moderate to severe chronic kidney disease | |
| asthma | |
| Drug therapy | long-term antidepressants |
| antiepileptics | |
| aromatase inhibitors | |
| long-term depot medroxyprogesterone acetate | |
| gonadotropin-releasing hormone agonists (in men with prostate cancer) | |
| proton pump inhibitors | |
| oral glucocorticoids | |
| thiazolidinediones | |
Scottish Intercollegiate Guidelines Network. Management of osteoporosis and the prevention of fragility fractures. SIGN 142. Edinburgh: SIGN, 2015 (updated 2020). Available at: www.sign.ac.uk/our-guidelines/management-of-osteoporosis-and-the-prevention-of-fragility-fractures/ Reproduced with permission | |
Diagnosis and Management
The updated SIGN guideline recommends that bone density scanning at the spine and hip based on a BMD cut-off T-score of −2.5 is the method of choice for diagnosis of osteoporosis. There is insufficient evidence to support the use of peripheral BMD measurements, ultrasound densitometry, or biochemical markers in the diagnosis of fracture risk. In addition, SIGN examined new evidence around screening, and concluded that it does not reduce fracture risk.1,11,12
Following diagnosis, the guidance recommends that the relevant treatment options are discussed with the patient, and that the patient’s views and preferences are taken into account. This consultation should include discussion of the risks of fracture with and without treatment, use of tools such as QFracture® and FRAX®, risks and benefits of treatment, and the option to decline drug treatment. Consideration should be given to the patient’s ability and motivation to adhere to different treatments. When recommending assessment and treatment, the patient’s life expectancy and the anticipated duration of treatment should also be considered.
Treatment of osteoporosis is targeted based on BMD measurements and the presence of clinical risk factors. Strategies for the management of osteoporosis focus on the prevention of fragility fractures using pharmacological and non-pharmacological interventions.
Non-pharmacological Interventions
Exercise of various types does slightly decrease the incidence of fracture and is recommended. A balanced diet is recommended, with additional vitamin D supplementation in winter in Scotland. Calcium and/or vitamin D supplementation is recommended for those whose dietary intake is insufficient, to reduce the risk of deficiency.1
Pharmacological Management
Pharmacological treatments that decrease the incidence of fractures include parathyroid hormones, such as teriparatide, alendronic acid, risedronate, zoledronic acid, ibandronic acid, denosumab, and hormone replacement therapy—Box 1 outlines the new recommendations on treatment in the 2020 update.1
| Box 1: New Recommendations on Pharmacological Treatments from the Updated SIGN Guideline on Management of Osteoporosis and the Prevention of Fragility Fractures1 |
|---|
Adapted from: Scottish Intercollegiate Guidelines Network. Management of osteoporosis and the prevention of fragility fractures. SIGN 142. Edinburgh: SIGN, 2015 (updated 2020). Available at: www.sign.ac.uk/our-guidelines/management-of-osteoporosis-and-the-prevention-of-fragility-fractures/ |
Side-effects of Treatment for Osteoporosis
There are some serious side-effects of bone building treatment, but these are rare. Osteonecrosis of the jaw and atypical femoral fractures do occur, and it is important that these risks are carefully shared with patients. Good oral hygiene is recommended during bisphosphonate therapy and patients starting bisphosphonates should be advised to have a dental check-up as soon as possible.1 Bisphosphonates can occasionally cause oesophagitis; patients should be informed about the need to swallow tablets whole with a full glass of water and the importance of remaining upright (seated or standing) for at least 30 minutes after taking the medication.1
Summary
Fragility fractures, especially hip fractures, cause substantial mortality and morbidity which manifests as pain and disability, as well as a great financial cost. Treatment with antiresorptive and anabolic medication prevents some of these harms and needs to be prescribed and maintained in patients at high risk from a fracture. The 2020 update to SIGN 142 includes new recommendations on risk factors and pharmacological treatments to support clinicians to deliver best practice in the management of osteoporosis and prevention of fragility fractures.
Dr David Stephens
GP, Scotland
Member of the SIGN 142 guideline development group
| Key Points |
|---|
DXA=dual-energy X-ray absorptiometry; SIGN=Scottish Intercollegiate Guidelines Network; NOGG=National Osteoporosis Guideline Group; BMD=bone mineral density |
| The Future of Osteoporosis Care |
|---|
Commentary from Dr David Stephens (NB this is not discussed in the update to SIGN 142) A fracture liaison service (FLS) is a bridge between secondary and primary care and is the most effective way of ensuring that patients with a fragility fracture start treatment promptly. CCGs and Health Boards where FLSs do not exist or are underdeveloped should put these in place to prevent further harm to their population. The RCP has an ongoing audit into the effectiveness of FLSs.13 With the advent of COVID-19, general practice is now much more a telephone and digital service. There is also less reliance on the GP, and more focus on a whole team approach. In future, a GP may not always be required to manage patients with osteoporosis who are moving back into primary care—a member of the primary care team, such as a practice pharmacist, advanced nurse practitioner, practice nurse, or musculoskeletal therapist, could take on this role. In addition, practices could appoint a Bone Health Lead to organise medication and review patients at 12–16 weeks, 12 months, and 3 years as stipulated by the NICE guidance,2 and provide the necessary support for patients with osteoporosis, especially when dealing with multimorbidity, polypharmacy, overdiagnosis, and concordance. |
| Implementation Actions for STPs and ICSs |
|---|
Written by Dr David Jenner, GP, Cullompton, Devon The following implementation actions are designed to support STPs and ICSs with the challenges involved with implementing new guidance at a system level. Our aim is to help you consider how to deliver improvements to healthcare within the available resources.
STP=sustainability and transformation partnership; ICS=integrated care system; ICS=integrated care system; NOGG=National Osteoporosis Guideline Group |
| Implementation Actions for Clinical Pharmacists in General Practice |
|---|
Written by Nicola Cree, Pharmaceutical Services Manager, Soar Beyond Ltd The following implementation actions are designed to support clinical pharmacists in general practice with implementing the guidance at a practice level. Osteoporosis management sits perfectly within the clinical pharmacist’s professional remit. Poor long‑term outcomes, coupled with poor adherence, offer pharmacists the prime opportunity to facilitate quality improvement in osteoporosis care.
Guidance and training for service development is available for a number of different clinical areas from Soar Beyond. If you have clinical pharmacists in your practice or organisation, contact Soar Beyond to see how they can support with clinical delivery, training, and development: soarbeyond.co.uk NHS England, NHS Improvement. Network contract Directed Enhanced Service: contract specification 2020/21—PCN requirements and entitlements. NHS England, March 2020. Available at: www.england.nhs.uk/wp-content/uploads/2020/03/network-contract-des-specification-pcn-requirements-entitlements-2020-21.pdf PCN=Primary Care Network; DES=Directed Enhanced Service |

