Dr Neelima Sibal and Mr Ajai Tyagi Present a Range of Patient Case Studies that Illustrate Different Causes of Red Eye and Suitable Treatment Options
| Read This Article to Learn More About: |
|---|
|
Patients with eye problems account for up to 5% of all general practice consultations.1,2 Red eye is a particularly common condition that is caused by inflammation or infection of the eye.2
Red eye can usually be managed effectively in general practice once the underlying cause has been determined. However, emergency referral to an ophthalmologist to rule out serious vision-threatening conditions is vital in some cases. Sometimes a lack of specialist equipment in the general practice setting can make it difficult to establish the correct diagnosis so specialist ophthalmological opinion may be required.2
A thorough history and physical examination will help to diagnose the cause of red eye.2
History Taking
NICE recommends that the history should include onset and duration of the symptoms and whether these are unilateral or bilateral. Other important associated features that also need to be assessed are changes in visual acuity, pain, foreign body sensation, discharge, and photophobia. It is worth asking about any history of contact lens use, trauma, or chemical exposure. A history of any similar previous episodes and medication should also be taken.3 Any relevant past medical history such as hypertension, inflammatory bowel disease, and connective tissue disorders may also inform the diagnosis of the eye condition.
Examination
Equipment that might be useful when examining the eye in general practice includes a Snellen chart, a light source, fluorescein eye drops, and cotton buds.4 Binocular magnifying loops and direct ophthalmoscopy might also be useful if clinicians have adequate training and experience in their use. A systematic eye examination based on the detailed history will help narrow the diagnosis and prevent missing any serious eye conditions.4
A stepwise examination may include an assessment of visual acuity, a thorough inspection of the eyelid and brow, orbit, conjunctiva, and cornea, an assessment of pupillary reactions, and swabs (see Table 1).
Table 1: Eye Examinations in Primary Care
| Type of Examination | What Should Be Included |
|---|---|
| Visual acuity | Visual acuity should be tested in both eyes and the patient asked whether they have noted any change in their vision. A reduction in normal vision may warrant urgent referral to an ophthalmologist to rule out serious conditions.4 |
| Lids and orbit | The lid and brow should be inspected to check for periorbital injury, lumps or swelling. Examination of the lid margin will reveal any matting of the eyelashes caused by discharge or crustations resulting from blepharitis. Orbital examination should uncover any orbital swelling or redness in cases of orbital cellulitis or orbital tumours.4 |
| Conjunctiva | Conjunctival examination should include the bulbar and tarsal conjunctiva. The upper tarsal conjunctiva can be examined by using a cotton bud to evert the upper eyelid. The pattern of redness on the conjunctiva will help with differential diagnosis, for example, segmental injection may suggest episcleritis, whereas generalised redness with tenderness of the globe on deeper palpation may suggest scleritis.3,4 If a foreign body is suspected, eversion of the upper eyelid may also help to uncover it.4 |
| Cornea | The cornea should be examined to investigate for haziness or the presence of foreign bodies. Fluorescein can be used to reveal any corneal abrasions or corneal ulcers.4 |
| Pupil | Pupillary reactions should be assessed using a pen torch or equivalent light source. The absence of pupillary response or irregularly shaped pupils in cases of red eye merit further referral to rule out sinister conditions such as anterior uveitis or angle-closure glaucoma.4,5 |
| Swabs | If conjunctivitis is suspected swabs should be undertaken for culture.4 |
Red Flags
NICE recommends urgent same-day assessment by an ophthalmologist or emergency referral for the following features, which may indicate serious underlying pathology for red eye presentation:3
- reduced vision
- deep pain in the eye or tenderness of the globe on palpation
- contact lens use
- high-velocity injury
- chemical eye injury
- fluorescein staining of the eye
- photophobia
- corneal foreign body
- distorted pupil
- neonatal conjunctivitis.
Recent ocular surgery may also be a cause of red eye.
The example case studies presented below discuss some of the causes of red eye that may be seen in general practice, along with their diagnosis and management.
Case 1
A 68-year-old man presents with sudden onset of redness of his left eye, which he first noticed on getting up in the morning. He has mild discomfort but there is no discharge from either eye. He cannot recall any history of trauma or foreign body. He says his vision is normal and he feels well in himself. On examination, his blood pressure is found to be 152/96 mmHg. Eye examination reveals a well-circumscribed area of confluent haemorrhage underneath the conjunctiva with a clearly visible posterior border. The cornea appears clear. Visual acuity and pupillary response are both normal. Fluorescein staining is negative.
Diagnosis
The most likely diagnosis in this case is non-traumatic subconjunctival haemorrhage (see Figure 1). This condition is benign and self-limiting unless it is caused by systemic factors.6,7
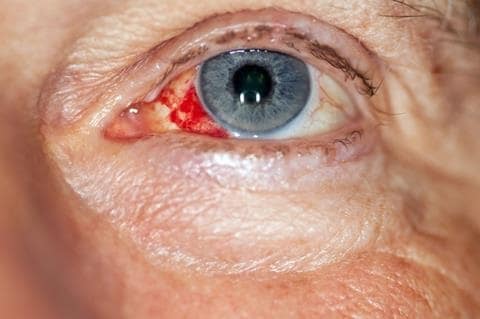
Burst blood vessel in the eye.
Source: NHS. Red eye. Available at: www.nhs.uk/conditions/red-eye/Contains public sector information licensed under the Open Government Licence v3.0.
Management
Unless underlying systemic illness is the likely cause, then the condition does not require treatment. Artificial tears may be used if the patient experiences mild irritation. Non-steroidal anti-inflammatory drugs and aspirin should be avoided because they can cause subconjunctival haemorrhage.6,7 The patient should be reassured about the benign nature of the condition, which can occasionally recur.
Clinical Outcome
The patient was reassured by the advice given and he took away detailed information including a written patient leaflet. The red eye settled down in 2 weeks.
Case 2
A 16-year-old female presents with sudden onset of ocular unease and redness of her left eye after returning home from school. She thinks something entered her eye when she was walking home. She also complains of a persistent scratching sensation, watering from the left eye and discomfort/pain that is worse on blinking. She says her vision on the left side is not as good as in the right eye. She does not wear contact lenses. On examination, her visual acuity is found to have reduced in her left eye to 6/12. The conjunctiva on the left side is injected with a normal pupillary reaction. There is no foreign body visible. The upper eyelid looks swollen, there is no discharge and fluorescein staining is positive.
Diagnosis
The likely diagnosis for this patient is corneal abrasion, where the cornea has been scratched or grazed (see Figure 2).8 It is important to make sure there is no foreign body retained on the ocular surface or under the upper eyelid to prevent further damage.2
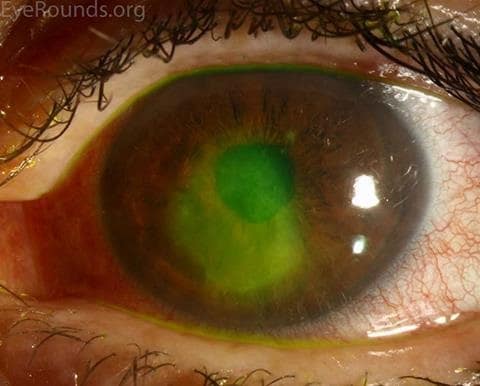
A corneal epithelial defect, or corneal abrasion, after the application of fluorescein dye.
Source: Vislisel J, Chan C. Corneal abrasion. EyeRounds.org, University of Iowa. Available at: webeye.ophth.uiowa.edu/eyeforum/atlas/pages/corneal-abrasion/index.htmReproduced with permission.
Management
Most cases of corneal abrasion can be treated with antibiotic treatment, lubricants at night, and cyclopentolate.
The cornea should heal after 2 or 3 days’ treatment with antibiotic ointment. It is recommended that an eye pad is used with antibiotic treatment to keep the eye closed and prevent irritation caused by blinking.8 However, some studies dispute the benefits of eye pads,2,9 so it is acceptable to use antibiotic eye drops without an eye pad.10
Lubricants should be used whenever the patient is sleeping, and will possibly be needed for a few weeks, to stop the eyelid sticking and causing further damage to the cornea.8
Cyclopentolate drops may be given to provide pain relief by dilating the pupil and relaxing the ciliary muscle. Patients should be advised that this will cause blurred vision for at least 12 hours so they should not drive or use machinery.8
Steroid preparations are contraindicated in patients with corneal abrasion.11
Clinical Outcome
The patient was advised to use topical chloramphenicol 0.5% eye drops every 4 hours in her left eye and an eye ointment at night. All her symptoms settled with this treatment and an ophthalmologist opinion was not needed.
Case 3
A 42-year-old man presents with redness of both eyes, which he has had for 4–5 days, and which initially started on the left side. He has some associated discomfort and sensation of having a foreign body. He does not complain of any problems with his vision. There is no itching but he has had purulent discharge for the last few days. On examination, diffuse injection of the conjunctiva is seen in both eyes with thick mucopurulent discharge noted in the medial canthus area of both sides and some dried secretions seen on the lashes. The cornea is found to be clear and fluorescein staining is negative. Visual acuity and pupillary responses are found to be normal.
Diagnosis
The patient has acute bacterial conjunctivitis (see Figure 3), the most common type of conjunctivitis seen in general practice.2 In adults, Staphylococcus aureus bacteria and in children, Streptococcus pneumoniae, Haemophilus influenzae, and Moraxella catarrhalis are common causative organisms.2,12
Symptoms of bacterial conjunctivitis may last for up to 4 weeks.2,12 Other types of conjunctivitis are hyperacute bacterial conjunctivitis, viral conjunctivitis, and allergic conjunctivitis.
Hyperacute bacterial conjunctivitis is a serious condition that is often caused by Neisseria gonorrhoeae in sexually active adults. Symptoms are copious purulent discharge, pain, and reduced vision, and there is a risk of corneal perforation, so urgent referral to an ophthalmologist is needed.2
Viral conjunctivitis may be associated with some discomfort, but the condition is usually mild and self-limiting, with symptoms generally only lasting for up to 2 weeks. Symptoms are irritation and watering of the eyes, but there is usually no purulent discharge. The condition may be highly contagious, especially if adenovirus is the culprit.2,10
Allergic conjunctivitis usually presents with itchy eyes and redness, and the condition is associated with allergic rhinitis, asthma, and/or eczema.2
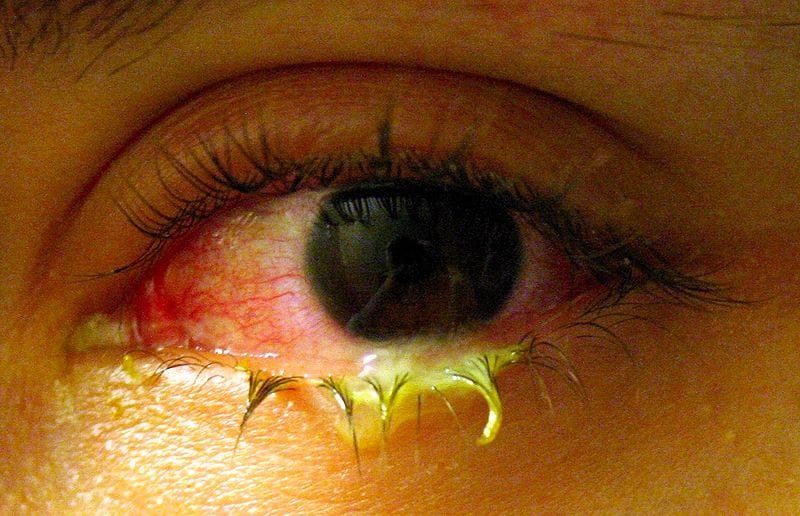
Source: Tanalai. Swollen eye with conjunctivitis. Available at: commons.wikimedia.org/wiki/File:Swollen_eye_with_conjunctivitis.jpgReproduced under the terms of the CC BY 3.0 license.
Management
Laboratory cultures should be used to identify bacteria in neonates, people who are immunocompromised, people who wear contact lenses, people with recurrent, severe, or chronic purulent conjunctivitis, or when the condition does not respond to initial treatment.2,13
Generally, topical antibiotics are prescribed for the treatment of bacterial conjunctivitis. However, just asking the patient to clean their eyes of the discharge may also be sufficient because this is a self-limiting condition.14 The NHS provides advice for patients on self-treatment for conjunctivitis (see www.nhs.uk/conditions/conjunctivitis).15
A Cochrane review of 11 randomised controlled trials showed that using antibiotic eye drops does modestly speed up the resolution of symptoms and infection.14 However, with worries about antibiotic resistance,16 it might be sensible to use delayed prescribing of antibiotic therapy, with antibiotics chosen according to their cost-effectiveness and local patterns of bacterial resistance.2
Clinical Outcome
In this case, a course of topical chloramphenicol 0.5% eye drops was advised for 5 days, which resolved the patient’s symptoms completely.
Case 4
A 48-year-old man who has previously been diagnosed with rheumatoid arthritis presents with left eye redness and pain. The symptoms came on suddenly and he also complains of the presence of a small spot in the area of redness. There is no eye discharge, headache, or vomiting. On examination there is localised sectorial redness in the lateral aspect of the left eye with a localised small nodule. There is no uptake on fluorescein staining. Visual acuity is found to be normal and pupillary reactions are equal and normal on both sides.
Diagnosis
Episcleritis is the likely diagnosis in this case, a common inflammation of the episclera, the layer of tissue between the conjunctiva and the sclera (see Figure 4). Symptoms are irritation and soreness that may be described as feeling gritty. The condition may recur and flare-ups may happen after a few months.17,18
Episcleritis may be caused by systemic inflammatory conditions such as rheumatoid arthritis, though in most cases no identifiable cause is found. It occurs more frequently in young adults through to people in their fifth decade.18
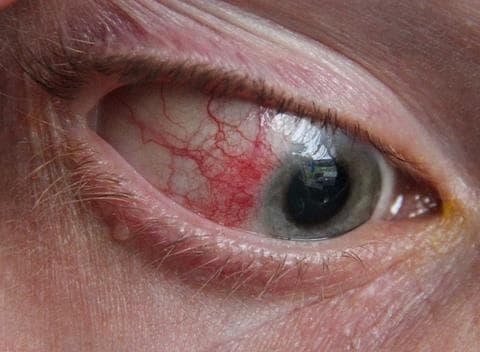
Source: Asagan. Episcleritis of eyeball. Available at: commons.wikimedia.org/wiki/File:Episcleritiseye.jpgReproduced under the terms of the CC BY-SA 3.0 license.
Management
Most cases of episcleritis do not require any further investigation but if there is suspicion based on clinical examination, then further biochemical tests should be arranged to rule out associated conditions like rheumatoid arthritis. Most cases of episcleritis are self-limiting and resolve in 7–10 days.18
Mild cases of episcleritis require no specific treatment. If the patient has significant eye discomfort then artificial tears can be used as necessary for 1–2 weeks.17 Patients should be reassured that the condition will not generally progress to a more serious eye problem, but they should return if their symptoms persist. Cold compresses can be used to relieve symptoms.19
Clinical Outcome
The patient was reassured, given detailed information about episcleritis including a written leaflet, and the presenting episode settled in 10 days.
Case 5
A 65-year-old Asian woman presents with sudden onset right-sided eye pain with redness. She also complains of vomiting and seeing halos around the light. She says that her vision in her right eye is not as good as in the left eye. No history of any ocular trauma is noted. Examination of her right eye reveals a mid-dilated pupil that is unresponsive to light, redness of the conjunctiva, and hardening of the left orbit on palpation. Visual acuity is found to be 6/12 in the right eye.
Diagnosis
The most likely diagnosis for this patient is acute angle-closure glaucoma (see Figure 5). This a serious vision-threatening condition that needs emergency referral. It is caused by a sudden blockage to the drainage in the eye, with an accompanying rapid increase in eye pressure.20 Emergency treatment is essential to avoid permanent loss of vision in the eye.
Acute angle-closure glaucoma is more common in:21
- people over 40 years old, particularly in those aged 60–70 years
- people with a close relative who has had acute glaucoma
- long-sighted people
- women
- people of Southeast Asian descent
- Inuit people.
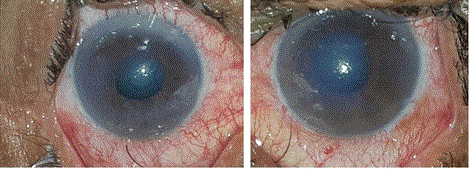
Slit-lamp photograph showing conjunctival injection associated with corneal oedema and mid-dilated pupil in both eyes.
Source: Mahmoud A, Abid F, Ksiaa I et al. Bilateral acute angle-closure glaucoma following tramadol subcutaneous administration. BMC Ophthalmol 2018; 18: 50.Reproduced under the BMC reprints and permissions policy.
Management
If acute angle-closure glaucoma is suspected, the patient should be referred immediately for specialist ophthalmology assessment and treatment.22
NICE recommends that if immediate admission is not possible, emergency treatment should be started in primary care:
- if the drugs are available, give: pilocarpine eye drops, one drop of 2% in blue eyes or 4% in brown eyes; acetazolamide 500 mg orally to reduce production of aqueous humour (provided that there are no contraindications); analgesia; and an anti-emetic, if required.22
Clinical Outcome
The patient was referred to the eye casualty at the local hospital, where her intraocular pressure was found to be raised at 55 mmHg (normal range 10–21 mmHg). Slit lamp examination revealed corneal oedema and a mid-dilated pupil, and gonioscopy of the fellow eye revealed closed angles of the anterior chamber. The patient was treated with intravenous acetazolamide 500 mg immediately, followed by tablets of acetazolamide 250 mg four times a day. A combination of topical anti-glaucoma eye drops were also used in the same eye, along with 2% pilocarpine eye drops in both her eyes (to prevent an acute angle-closure glaucoma in the fellow eye). A few days later she underwent bilateral YAG laser peripheral iridotomies to prevent any further episodes of acute angle-closure glaucoma.
The patient did fully recover her vision because she had been referred urgently to the eye casualty for the treatment.
Conclusion
Red eye is a common presentation and in most cases is caused by relatively benign conditions, which can be managed in general practice. A small proportion of cases have a serious underlying cause and can be sight-threatening, requiring urgent, specialist assessment and input.
Dr Neelima Sibal
GP Partner, Oakham Surgery, Your Health Partnership
Mr Ajai Tyagi
Consultant Ophthalmologist and Vitreoretinal Surgeon, Sandwell and West Birmingham NHS Trust

